Practice of Telemedicine: Legal Considerations
The developments in the information technology coupled with the increased access to smartphones in rural areas led to the recognition of the benefits that telemedicine offers. The concept of telemedicine gained popularity, especially for the reason that it helps in providing medical services to persons with little or no access to healthcare facilities. The COVID pandemic also led to development of telemedicine services
Telemedicine plays an important role in cases where there is no need for the patient to physically visit the medical professionals, e.g. for regular, routine check-ups, for continuous monitoring, or for nutritional related advice. However, in the absence of proper regulations, there were certain issues relating to medico-legal implications of telemedicine, including registration, licensing, insurance, quality, privacy and confidentiality. Therefore, in March 2020, the Ministry of Health and Family Welfare notified the Telemedicine Practice Guidelines by way of an amendment in the Indian Medical Council (Professional Conduct, Etiquette and Ethics) Regulations, 2002. The guidelines lay down the policy framework on various aspects of telemedicine including information on integration of technology platforms and tools to provide health care delivery. These guidelines are not in supersession of existing standards and protocols and therefore, have to be interpreted in conjunction with the national clinical standards, protocols, policies and procedures.
Telemedicine services include sharing and transfer of medical information and expertise through information and computer technological modes, with the aim to facilitate diagnosis, treatment, and management of patients.
Need for Telemedicine Regulations
The foremost issue was the inadequate quality of healthcare services, especially in the rural areas on account of reluctance of qualified medical practitioners to settle in rural areas.
Secondly, the Bombay High Court, in the case of Deepa Sanjeev Pawaskar and Anr. v. State of Maharashtra, 2018 SCC Online Bom 1841, held the applicants (two doctors) liable for medical negligence for the medical consultation provided though telephonic medium. After the judgement of the high court, medical professionals were hesitant in practicing telemedicine.
Further, disasters and pandemics, including the Covid-19 pandemic, pose unanticipated challenges to the healthcare framework in India, including the growing lack of healthcare professionals who are currently engaged at the forefront dealing with infected persons needing medical attention. In such dire circumstances, telemedicine services are a boon, which can aid in containing the health crisis, by ensuring widespread services and reducing chances of infecting other persons, including the medical professionals themselves.
The lack of legal framework in this regard was a hindrance in the growth of the telemedicine sector. The Telemedicine Practice Guidelines of 2020 (the “Guidelines”) is an attempt to fill in the void in the legal framework for practice of telemedicine.
Brief Overview of the Guidelines
The guidelines permits the medical professionals to provide consultation services through telecommunication and computer technologies. The consultations with a patient may be done on real time basis, like video-calls, or asynchronous basis, like through transmission of summary of patient complaints and supplementary data including images, lab reports and/or radiological investigations between stakeholders. The RMPs can provide emergency consultation or non-emergency consultation, including first check-up and follow ups. All of this provides considerable flexibility to the medical professionals.
The guidelines also recognized the role played by the technology platforms in enabling telemedicine and therefore, laid down certain important obligations for the technology platforms.
Guidelines for Medical Professionals
Mandatory online course on Telemedicine
In order to enable all the interested medical professionals to get familiar with these Guidelines as well as with the process and limitations of telemedicine practice, the National Medical Commission will develop an online program. All registered medical practitioners intending to provide online consultation through telemedicine would be required to complete the mandatory online course within three (3) years of its notification. Till the notification of this course, the principles mentioned in the guidelines have to be followed. After three (3) years from the notification of the course, undergoing and qualifying such a course would be essential prior to practice of telemedicine.
Till October 2021, no such course has been notified.
Patient Verification and Consent
The medical professional is obligated to disclose his name and qualification to patient. He must display his medical council registration number on prescriptions, website, electronic communication (WhatsApp/ email etc.) and receipts etc. given to his/her patients. The medical professional should also verify the patient’s identity, like name, age, address, email address, phone number, registered identification or any other appropriate identification. Minors can also avail tele-consultations but only when such consultation is in presence of an adult whose identity details have been verified.
In cases wherein a patient initiates telemedicine, the patient’s consent is implied by his actions. However, in an instance, wherein the tele-consultation is initiated by another RMP, health-worker or caregiver, then the patient’s explicit consent needs to be obtained from the patient through email, text, audio or video message, and the same has to be recorded in patient records.
Prescription and Preservation of Record
It is mandatory to provide the patient a digital copy of the signed prescription or e-prescription through e-mail or any messaging platform. If the medical professional transmits the prescription directly to the pharmacy, then such professional must obtain the explicit consent of the patient that entitles him/her to get the medicines dispensed from any pharmacy of his/her choice
It is important to maintain, for such period as prescribed from time to time, log or record of telemedicine interaction such as phone logs, text records, video interaction logs etc. Also the patient records, including explicit patient consent, case history, investigation reports, images, etc., and prescription records must be maintained. For preservation of medical records, the time of three (3) years prescribed for preservation of records of indoor patients can be considered as a benchmark.
Fee for Consultation
The medical professionals can charge appropriate fees for tele-consultation in the same way as done for in-person consultations. Moreover, the receipt/invoice for the fees charged for tele-consultation to the patient should also be provided in a similar manner.
Medicines that can be prescribed
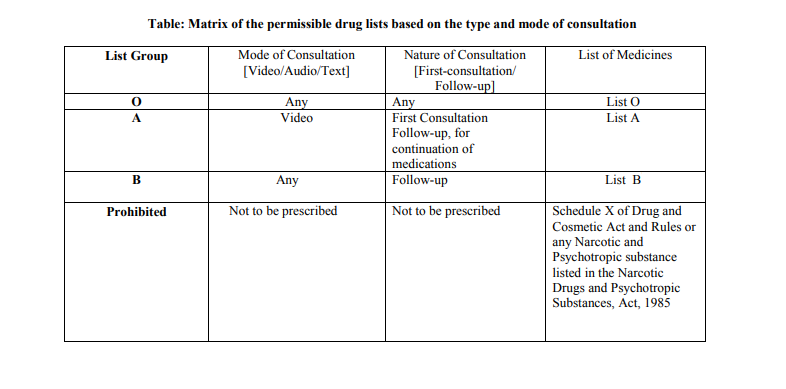
The guidelines classified various medicines, which can be prescribed via teleconsultation in different groups on the basis of mode and nature of consultation.
- List O – This list comprises over the counter medicines and medicines notified by the Central Government during public health emergencies, and they can be prescribed through any mode of tele-consultation.
- List A – This list in inclusive of medicines that can be prescribed during the first consult which is a video consultation and are being re-prescribed for re-fill, and those which are considered relatively safe with low potential for abuse.
- List B – This list includes medicines that can be prescribed to a patient who is undergoing follow-up consultation along with medicines that have been prescribed during in-person consultation for the same medical condition.
- Prohibited List – This list is inclusive of medicines that an RMP cannot prescribe during tele-consultation, as they have a high potential of abuse and could harm the patient or the society at large if used improperly.
Professional ethics and standards
All medial professionals are bound to uphold the same professional and ethical norms and standards as applicable to traditional in-person care, within the intrinsic limitations of telemedicine. The medical professionals must abide by the principles of medical ethics, including professional norms for protecting patient privacy and confidentiality as per the Indian Medical Council Act, 1956.
Markedly, the following actions on part of the medical professionals are not permissible:
- Insisting on tele-consultation against the patient’s wishes.
- Misuse of patient images and data.
- Prescribing medicines from prohibited list.
- Solicits patients for telemedicine through any advertisement or inducement.
Guidelines for Technology Platforms
Only registered medical professionals to be listed on platform
The technology platforms have to ensure that the medical professionals providing tele-consultations are registered with the national medical council or the state level medical councils. They must conduct their due diligence before listing any medical professional on their portal. The platform is also required to provide the name, qualification and registration number, contact details of all the medical professional listed on the platform.
Use of artificial intelligence or machine learning
Technology platforms cannot use artificial intelligence or machine learning to counsel patients or to prescribe medicines to patients. The registered medical practitioner must directly communicate with the patient for counselling and prescription of medicines.
However, artificial intelligence, machine learning, advanced data science-based decision support systems etc. can be used by the technology platforms to assist and support the RMP regarding patient evaluation, diagnosis or management, but the final counselling or prescription would have to be given by the medical professional.
Grievance Redressal Mechanism
Technology Platforms have to ensure that there is a proper grievance redressal mechanism for addressing queries and for redressal of grievances of the end-customer. Technology platforms are also bound to report all non-compliances to the National Medical Commission.
Penalty for non-compliance
If any technology platform is found in violation of these guidelines, the National Medical Commission can blacklist such platform. The registered medical practitioners have been barred from providing telemedicine services on any blacklisted technology platform.
Concluding Remarks
The guidelines had elaborately laid down the codes of conduct for medical professionals for providing services through telemedicine. The guidelines have also recognized the role of technology platforms in enabling telemedicine.
The notification of the guidelines is a welcome step, especially considering the current scenario of COVID-19. These guidelines have the potential to make instrumental positive changes in the healthcare sector as the challenges concerning the access and quality issues can be addressed by telemedicine to a greater extent.
•Laws are constantly changing, either
their substance or their interpretation. Even though every attempt is made to keep the information correct
and updated, yet if you find some information to be wrong or dated, kindly let us know. We will acknowledge
your contribution.Click here to know more.
•Disclaimer: This is not professional advice. Please read Terms of Use (more specifically clauses 3 and 4) for detailed disclaimer.